Article Text
Abstract
Background A minority of patients make frequent and excessive calls to the ambulance service, placing a significant burden on limited resources at a time when demand on urgent and emergency care systems is steadily increasing. Little is known about the reasons underlying frequent caller behaviour or the best way to manage this group of patients.
Objectives The present study aimed to (i) profile frequent callers to the ambulance service and (ii) evaluate the impact of a case management interventional approach on frequent caller behaviour.
Methods A retrospective review of data from a 2-year period (from 1 April 2009 to 31 March 2011) was conducted. Patients were included in the analysis if they had been accepted for case management intervention by the Patient-Centred Action Team during this period and met the study inclusion criteria.
Results The review identified 110 frequent callers who met the study inclusion criteria. The majority of frequent callers (86%) had multiple and complex reasons for calling, including frequent medical need, acute or chronic mental health condition, older age and unmet personal or social care needs. In the majority of cases (82%), multiple interventional strategies were required. A significant reduction in median call volume was observed from preintervention to postintervention (from five calls/month to zero calls/month).
Conclusions Effective management of this complex patient group requires an individualised case management approach in order to identify and tackle the underlying causes of behaviour.
- emergency ambulance systems
- prehospital care
Statistics from Altmetric.com
Key messages
-
What is already known on this subject
-
Several recent studies have attempted to characterise frequent callers to the ambulance service with regards to chief complaint at the time of patient presentation. However, frequent callers may present with multiple complaints on each occasion that they call 999 and little is known about the underlying causes of frequent calls to the ambulance service. The evidence regarding the best way to manage this patient group is confined to one pilot study limited by a very small sample size.
What this paper adds
-
This study found frequent callers to have complex underlying unmet medical, mental health, social and personal care needs. An individualised case management programme was associated with reduced call volume.
Introduction
Demand on emergency and urgent care systems in the UK has been steadily increasing at an estimated rate of 6.5% per year, which equates annually to an additional 300 000 calls at an approximate extra cost of £60 million.1 A range of urgent care services exists, including walk-in centres, minor injury units, general practitioner (GP) surgeries including out-of-hours services, NHS Direct and, more recently, 111. However, significant inappropriate use of the ambulance service is reported, with estimates ranging from 16% to 52%.2 A study of 300 consecutive patients conveyed by the London Ambulance Service (LAS) to one London hospital reported that for only 53.7% of cases was the reason for calling an ambulance deemed to be appropriate.3
A number of recent studies have attempted to investigate why people call for an emergency ambulance. A qualitative study of patients who called 999 for a condition that could have been treated in primary care4 suggested a number of reasons including perceived or actual barriers to accessing urgent care services, previous negative experience of urgent care services, the perception that the ambulance service could provide rapid triage and assessment, patient and carer anxiety, and carers’ feelings of responsibility and helplessness. Other reasons centre around a lack of awareness of alternative services, lack of transport to reach the emergency department (ED) and the wish to avoid a long wait in ED.3
In addition to patients who call on a single occasion when a more appropriate urgent care service is available, there are a minority of patients who make frequent and excessive calls to ambulance services, accounting for a disproportionate volume of calls.1 The LAS defines a frequent caller as an individual who has called the ambulance service 10 times per month for 3 months and/or where the quantity of calls is considered to have a significant impact on LAS resources.5 The cost to the LAS of each emergency ambulance journey to an ED is £255, with further costs of £8 per call, £65 per patient receiving clinical telephone advice and £155 per patient seen but not conveyed.6 Patients conveyed to ED will incur further attendance tariffs ranging from £59 to £237.7 Frequent callers to the ambulance service may also make repeated calls to, and attend, other urgent and primary care services (e.g. ED, GP practice, out-of-hours services) and also other emergency services including the police and fire service,5 although the extent to which this occurs is unknown.
Although recent studies have investigated reasons behind frequent attendances at ED and why people in general call 999 on a single occasion, there exists little literature examining reasons behind frequent calls to ambulance services.8 One US study found frequent callers to an ambulance service to be characterised by male gender, black ethnicity, age over 35 years (particularly 45–54), behavioural health problems and chronic conditions including asthma and diabetes.9 A study of elderly patients requiring frequent conveyance to ED reported similar patient characteristics and also cited homelessness and number of conditions/medications as factors predictive of high use.10 Another US study investigated repeat ambulance use by paediatric patients (aged 0–21 years) requiring conveyance to ED.11 Almost half of the repeat calls were related to patients aged 17–21 years, with repeat calls associated with a chief complaint of seizure, assault, suicide attempts, abdominal/chest pain, pregnancy and mental/behavioural problems. However, as noted by Scott et al,8 the majority of the studies that have been conducted have focused on patients who were conveyed by ambulance, meaning that those who were not conveyed or who were not sent a response were excluded. Indeed, of three studies described above, only the first study9 included all frequent callers to the ambulance service, irrespective of whether they were conveyed.
A recent study by Scott et al12 characterised the top 100 frequent callers to the Yorkshire Ambulance Service over a 1-year period. Frequent callers were found to be a heterogeneous group. When compared with the rest of the population, frequent callers were more likely to be assigned call codes of abdominal pain/problems, breathing problems, chest pain (non-traumatic), psychiatric/abnormal behaviour/suicide attempt, sick person, headache, unassigned and falls. Frequent callers were more likely to call before 9am or after 4pm—when primary care or community services may have been unavailable—and were more likely to be allocated a lower urgency response. However, frequent callers may present with multiple complaints when calling 999—but only one complaint is assigned a call code—and the chief complaint may vary each time they call. Thus, while examining the chief complaints of frequent callers provides useful information, it does not allow the identification of the underlying cause of frequent calls to the ambulance service, which is essential to understand frequent caller behaviour and devise appropriate interventions.
Better management of frequent callers may reduce costs, free-up clinical resources and improve the quality of patient care. Patient-Centred Action Team (PCAT) employs a variety of approaches to manage the behaviour of frequent callers, depending on the patient's needs and behaviour. However, little evidence exists regarding the best way to manage this patient group other than one US pilot study—limited by a small sample size (n=10)—which reported that weekly case management visits over a 5-week to 12-week period resulted in a reduced number of ambulance responses.13 The impact of UK ambulance services’ frequent caller management strategies—such as those used by the LAS PCAT—on frequent caller behaviour has not been previously investigated.
Our study had two aims:
-
to generate a profile of the LAS’ frequent callers;
-
to examine the impact of the LAS PCAT's interventions on frequent caller behaviour, specifically call volume.
Methods
Study setting
The LAS serves the area of Greater London, which spans an area of approximately 620 m2 populated by 8.2 million people. Each year, the LAS receives 1.6 million calls and attends more than one million incidents.14
LAS PCAT procedure
Frequent callers to the LAS are managed by PCAT, which aims to identify the underlying cause of the patient's behaviour and implement a care plan that reduces call volume to the LAS while ensuring the patient's well-being.5 PCAT categorises frequent callers using the following profile categories: high levels of anxiety, perceived need for attention, chronic/acute mental illness, substance abuse, frequent fallers, frequent clinical/medical need, failure to understand the role of the ambulance service, unmet social/personal care needs, specific behavioural conditions and ignorant/malicious hoaxers.15 However, the distribution of patients among these profile categories is unknown.
Two methods are currently used for identifying frequent callers to the LAS. Ambulance clinicians may refer patients who they think are frequent callers to PCAT by completing a designated referral form. Additionally, data are captured by the LAS Management Information (MI) department comprising call volume from specific telephone numbers. This information is sent to PCAT who review the data to identify frequent callers. Following a referral or identification using MI data, the call volume for the previous 12 months is examined. The decision regarding whether to accept the case for intervention is based on (i) call volume (i.e. whether it is high enough to place a significant impact on LAS resources), (ii) unusual pattern of calls/chief complaint, and (iii) location of calls, for example, care home. Current PCAT practice defines frequent callers as patients who have called the ambulance service 10 times per month for 3 consecutive months or patients who have a high call volume that does not meet the threshold but whose behaviour suggests that they are at risk to themselves and/or of using significant ambulance service resources. However, as this practice for defining frequent callers was put in place relatively recently, some of the patients included in the present study do not meet these criteria but were accepted based on referrals made from ambulance clinicians or external organisations (e.g. local EDs).
Intervention
Once a referral has been accepted by PCAT, the patient may be sent an ‘approach letter’ informing them that they have been identified as a frequent caller and advising on appropriate use of NHS services. Contact may be made with the patient's GP and agencies, including social services, community mental health team and the police. Multiagency meetings may be held to gain information on the patient's medical and mental health, social background and to identify any issues with the patient's primary or community care. Other available interventions involve the creation of an individual dispatch protocol (IDP) or patient-specific protocol (PSP). An IDP informs the emergency medical dispatcher of the appropriate action to take when responding to 999 calls from a particular patient or address. PSPs are created where the treatment required falls outside of standard practice for a particular condition and specify the treatment to be given to a named patient by the attending ambulance clinicians. Finally, case reviews are undertaken for all patients identified as frequent callers. The reviews involve examining call volume for each patient and assessing their care plan to identify escalations in call volumes, whether patients are responding to their care plan and to ensure that resources are targeted appropriately and priority for case management reviewed.
Cases are closed when the patient's call volume has decreased to an acceptable level based on their individual circumstances or if the patient is deceased, has been incarcerated, moved out of the catchment area of the LAS or is untraceable.
Participants
Patients were included in the analysis if they were entered on the database used by PCAT during the period 1 April 2009 to 31 March 2011 and if the following information was available: duration of case management, first referral date, date the file was closed and initial call volume and behaviours.
Data collection procedure
Data were extracted from the database for patients meeting the criteria specified above. Information was collected on patient demographic characteristics (age, gender), patient profile category as determined by PCAT (e.g. chronic/acute mental illness, substance abuse), number and types of intervention employed, the duration the case was open, call volume, whether the case was reopened and length of time between the case being closed and reopened. The types of interventions administered were graded on a scale from 1 to 4 based on the level of intensity of the intervention. Grade 1 interventions comprised the evaluation of patient behaviour with 6-weekly review and were applied to all patients deemed to be frequent callers. Grade 2 interventions included contacting the patient and/or the patient's GP. Grade 3 interventions included contact with social services, community mental health teams, the police and other agencies. Grade 4 interventions included multiagency meetings and the creation of IDPs and/or PSPs.
Outcome measures
To measure the effectiveness of PCAT practice, call volume preintervention and postintervention was measured. For most patients, preintervention call volume was taken from the 3 months prior to the case being opened. For a minority of patients, the preintervention period was shorter than 3 months, that is, cases where patient referrals were accepted on the basis of a very high call volume over a period of 1 or 2 months or due to a referral from an ambulance clinician or external organisation. Postintervention call volume was taken from the 3 months after the case was closed. To adjust for differences in the preintervention duration, a preintervention and postintervention call volume ratio was calculated by dividing the total number of calls by the number of months. Change in call volume ratio was the primary outcome measure.
Statistical analysis
Descriptive statistics were used to describe the frequent callers’ profile and the type and number of interventions received. A Wilcoxon test was used to compare call volume ratio preintervention and postintervention as the data were not normally distributed. A p value of <0.05 was considered significant. Statistical analyses were performed using SPSS V.19.
Results
Participants
The final sample included 110 patients. The mean age of the frequent callers was 57.6 years (SD=21.4, range=15–98). Just under half of the sample were men (n=49; 45%).
Profiling of frequent callers to the LAS
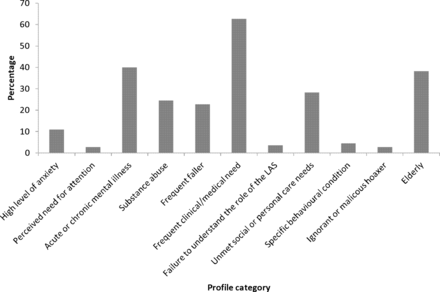
Eleven categories were used to profile frequent callers (figure 1). Categories were not mutually exclusive so more than one category could apply to each patient. Eighty-six per cent of patients (n=95) had more than one profile category applied to them, with 44% of patients (n=48) having two categories, 33% (n=36) having three categories, 7% (n=8) having four categories and 3% (n=3) having five categories applied to them. The most frequently occurring profile category was frequent clinical/medical need (n=70; 64%), followed by acute or chronic mental illness (n=44; 40%), elderly (n=42; 38%) and unmet social/personal care needs (n=31; 28%). Additionally, 16.4% of patients (n=18) had suicidal intentions/self-harm as their presenting complaint.
Profiles of frequent callers to the London Ambulance Service (LAS). More than profile category could be applied to each patient, thus percentages do not equal 100.
PCAT intervention: type, number and intensity of interventions received
The types of intervention received by frequent callers are displayed in figure 2. All patients (n=110) received monitoring of behaviour with 6-weekly review (grade 1). GPs were contacted in just over half (n=67; 61%) of all cases (grade 2), while contact with other agencies was made in just over one-quarter of cases (n=31; 28%; grade 3) and multidisciplinary case conferences were held for just under one-fifth of cases (n=19; 17%; grade 4).
Type of intervention received by frequent callers. Patients could receive more than one type of intervention, thus percentages do not equal 100. GP, general practitioner.
Eighty-three per cent of patients (n=91) received more than one different type of intervention. Half of the patients (n=56; 51%) received two types, with 21% (n=23) receiving three types, 5% (n=5) receiving four types, 6% (n=6) receiving five types and 1% (n=1) receiving six types of intervention.
PCAT intervention: evaluation of intervention on patient behaviour
The median duration that cases were open was 5.8 months, although there was wide variation from 0 to 24.3 months. Median preintervention call volume was 5 calls/month (range=0.6–24.5). Median postintervention call volume was 0 calls/month (range=0–8.0). A Wilcoxon test indicated call volume was significantly reduced from preintervention to postintervention. Eight per cent of closed cases were subsequently reopened during the study period due to an increase in call volumes. The median time between cases being closed and subsequently reopened was 7 months (range=2–29).
Discussion
Frequent callers to the ambulance service appear to be a heterogenous group, consistent with the findings of previous studies.12 Similarly, there is a striking similarity between the profiles of frequent callers to the ambulance service and frequent users of the ED.16 Most patients received more than one type of intervention, with over 30% of patients receiving three or more types of intervention. This highlights the complexity involved in managing this group of patients and the need to adopt an individualised approach that tackles the underlying cause of the frequent callers’ behaviour—be it a medical, mental health, social or personal care need. Studies of frequent ED users have similarly identified the need for individualised and multiple inventions, with a systematic review concluding that case management can reduce frequent ED use, decrease ED costs and has the potential to improve health and social outcomes.17
A significant decrease in call volume was observed from preintervention to postintervention, suggesting that the PCAT intervention strategy appears to be effective in reducing excessive and unnecessary calls to the ambulance service. Although this study did not look at the impact on costs, a reduction in call volume from a median of five calls per month to zero calls per month for this patient group is likely to be associated with a significant reduction in costs related to call handling, clinical telephone advice, ambulance clinician assessment and treatment—with or without conveyance—and attendance at ED. A reduction in call volume will also have the benefit of ‘freeing up’ valuable resources required to provide an effective service for patients who genuinely require an emergency ambulance. Eight per cent of closed cases were subsequently reopened during the study period. Given the complexity of the patient group and that a large number of frequent callers may have behaviours that fluctuate, it is expected that some may experience a crisis following case closure and begin to make calls again.
Without collecting data on the impact on costs—which was outside the scope of the project—we are unable to determine the cost-effectiveness of the programme, which cost approximately £410 000 to run during the study period. However, studies of case management interventions for frequent ED users have found the cost of case management is outweighed by reductions in ED costs in many cases.17 Thus, considering the cost per call to the ambulance service, the cost of providing a response (telephone advice or face-to-face) and costs to the ambulance service and ED should the patient be conveyed, we would expect the cost of the case management approach employed to be outweighed by the cost savings to the ambulance service and local hospitals.
The main limitation of the study is the lack of a control group. We cannot be certain that reductions in call volume were due to the interventions employed and did not reflect coincidental changes in patient behaviour. Given the typically chronic and complex nature of the underlying causes of frequent callers’ behaviour, it seems unlikely that significant reductions in patient contacts would occur spontaneously. Studies of frequent ED users suggest regression to the mean; only a minority of patients remained frequent attenders and this proportion decreased each year.18 ,19 However, these studies defined frequent users as those attending ED 2–10 times per year—which is considerably lower use than the 10 calls per month criteria used by PCAT—and the studies used a longer follow-up period. One further study of frequent ED users reported that 56% of patients who met the frequent user criteria for 2 years continued to use ED frequently,20 which led to the suggestion that there may be a subgroup of chronic frequent users.16
The impact of PCAT interventions on patient well-being was not investigated. The profiling of these patients suggests many of these patients repeatedly call the ambulance service due to unmet medical, mental health, social or personal needs. We speculate that the reduction in call volume may represent an improvement in patients’ needs being met through primary or community-based services as a result of PCAT interventions involving contacting GPs and other agencies. Educating frequent callers about appropriate use of the ambulance service and availability of more appropriate services may also have contributed to the reduction in call volume. However, the importance of improving care for this group of patients should not be underestimated, particularly as they may be failed or neglected by other health services. Future evaluations of the management of frequent callers should examine the impact on patient well-being and also include a control group. Engaging frequent callers in research is likely to be difficult, but future research investigating reasons behind frequent calls to the ambulance service should also consider the patient's perspective.
Forty per cent of frequent callers were categorised as having acute/chronic mental health issues and 16.4% of patients had suicidal intentions/self-harm as their presenting complaint. This is consistent with the previous literature, which suggests that one characteristic of frequent callers to the ambulance service may be presenting complaints related to suicide, psychological and/or behavioural problems.9 ,11 ,12 The high proportion of calls from patients with mental health problems may be due to patients experiencing particular difficulties in accessing appropriate community-based services and/or comorbidities with chronic physical health conditions since an estimated 46% of people with a mental problem have a chronic physical condition.21
Given the complexity of the patient group and the effectiveness that we are able to demonstrate of an individualised approach to case management, greater investment and resources are recommended for the management of this patient group. Many of the patients included in the study did not meet the PCAT criteria of 10 calls per month and were accepted for case management on the basis of either a referral from an ambulance clinician or external organisation, or due to a large number of calls in a shorter time period (e.g. a patient with a mental health condition experiencing an episodic crisis). Increasing resources would allow the management of patients with a lower call volume, which may be beneficial to both patient well-being and the ambulance service.
In conclusion, frequent callers to the ambulance service are a diverse group of patients with complex needs, who require an individualised approach to identify and tackle the cause(s) of their behaviour. The interventional approach used by the LAS PCAT is associated with reduced call volume from frequent callers, which is likely to be associated with reduced costs to the ambulance service, freeing up of resources to respond to other patients and improved patient well-being. Future research should examine the impact of effective management of frequent caller behaviour on health service costs and also explore the patient's perspective, particularly, the impact on patient well-being.
Acknowledgments
We would like to thank John O'Keefe for his input into the design of the project and Dr Vernie Balasubramaniam for her assistance with data collection.
References
Footnotes
-
Contributors MJE was involved in the conception, design, analysis, interpretation of data and drafting the article. GB was involved in the conception of the study and critically reviewing the manuscript. LS was involved in the design, interpretation of data and critically reviewing the manuscript. RTF was involved in interpretation of data and critically reviewing the manuscript. All authors provided final approval of the version to be published.
-
Competing interests None.
-
Ethics approval London Ambulance Service NHS Trust R&D office.
-
Provenance and peer review Not commissioned; externally peer reviewed.