Article Text
Abstract
Background Prehospital identification and selection of treatment strategy in patients with suspected non-ST-elevation myocardial infarction (NSTEMI) is challenging. The aim of this study was to evaluate the feasibility and diagnostic accuracy of prehospital ECG, troponin T (TnT) and transthoracic echocardiography (TTE) acquired by paramedics in early identification of NSTEMI.
Methods Consecutive patients requesting an ambulance from Sorlandet Hospital, Norway due to chest pain between November 2017 and January 2020 were screened for inclusion in the study. One ambulance was equipped with ECG recorder, point-of-care TnT test and TTE scanner, and six paramedics were given necessary training. ECG, TnT result and TTE images were acquired prehospitally and transferred to an in-hospital cardiologist. NSTEMI was suspected in patients with ischaemic ECG changes, elevated TnT or myocardial regional wall motion abnormalities (RWMA) at TTE.
Results A total of 253 patients were included in the study. ECG was interpretable by cardiologists in 243 (96%), TnT in 238 (94%) and TTE images in 240 (95%) patients. NSTEMI was the discharge diagnosis in 22 (9%) of these patients. Four (18%) patients with NSTEMI had ischaemic ECG changes, elevated TnT and RWMA at TTE. Eight (36%) patients with NSTEMI had positive findings at two of the diagnostic methods, six (27%) patients had positive findings at one, and four (18%) patients had no positive findings in any of the diagnostic methods. In three patients (14%) with NSTEMI, RWMA was the only positive test. The negative and positive predictive values for RWMA were 42% and 96%, respectively.
Conclusions Prehospital acquisition of ECG, TnT and interpretable TTE images by paramedics were feasible in most patients with chest pain. Based on these examinations, it was possible to identify the majority of cases with NSTEMI prehospitally and admit the patients directly to a hospital with facilities for percutaneous coronary intervention (PCI) for further treatment.
Trial registration number NCT04223986.
- acute myocardial infarct
Data availability statement
Data are available on reasonable request. The data that support the findings of this study are available on request from the corresponding author (JJ). The data are not publicly available due to state restrictions.
This is an open access article distributed in accordance with the Creative Commons Attribution 4.0 Unported (CC BY 4.0) license, which permits others to copy, redistribute, remix, transform and build upon this work for any purpose, provided the original work is properly cited, a link to the licence is given, and indication of whether changes were made. See: https://creativecommons.org/licenses/by/4.0/.
Statistics from Altmetric.com
Key messages
What is already known on this subject
ECG, troponin and transthoracic echocardiography (TTE) are important diagnostic tools for identification, risk stratification and timing of treatment in patients with non-ST-elevation myocardial infarction (NSTEMI).
Today the prehospital risk stratification is primarily based on a 12-lead ECG which has limited sensitivity in identifying NSTEMI.
What this study adds
This prospective study revealed that prehospital ECG, troponin and interpretable TTE images acquired by paramedics were feasible in most patients with suspected NSTEMI.
The diagnostic accuracy of the combination of these tests was sufficient for cardiologists to identify the majority of cases with NSTEMI prehospitally.
A prehospital diagnosis of NSTEMI may facilitate transport of these patients directly to a PCI hospital for earlier treatment.
Introduction
Chest pain is a frequent cause of contact with the healthcare system and has a wide array of possible aetiologies.1 2 Only a small proportion of these patients have an acute myocardial infarction (MI).1 3 However, early revascularisation is recommended to minimise irreversible myocardial damage and improve outcome caused by an acute coronary occlusion in most patients with MI.4 5 Prehospital risk stratification in patients with chest pain is challenging. In Norway, the initial evaluation is usually performed at first contact with the emergency medical service in the prehospital setting by ambulance paramedics, and the risk stratification is primarily based on a 12-lead ECG. However, the 12-lead ECG has limited sensitivity in identifying MI without ST-elevation and >30% of the patients with non-ST-elevation myocardial infarction (NSTEMI) have a normal ECG.5 6
Biomarkers, preferably cardiac troponin, are central in defining MI.7 Point-of-care tests (POCTs) of cardiac troponin applied in the prehospital setting may be useful in identifying MI.8 9 Out-of-hospital use and shorter turnaround time are the main advantages, but POCTs have lower sensitivity, lower diagnostic accuracy and lower negative predictive value than traditional methods. Additionally, cardiac and non-cardiac pathologies other than MI, may result in myocyte injury and elevated troponins.
European Society of Cardiology (ESC) guidelines recommend routine transthoracic echocardiography (TTE) by a trained physician in the ED in all patients with non-ST-elevation acute coronary syndrome (ACS).5 Myocardial regional wall motion abnormalities (RWMA) (ie, segmental hypokinesia or akinesia) are suggestive of myocardial ischaemia or necrosis, but this examination requires both advanced ultrasound equipment and considerable expertise and experience to interpret the findings.10–13 Consequently, the experience with prehospital TTE is limited.14 15 The feasibility of a diagnostic evaluation of patients with suspected non-ST-elevation ACS by paramedics using a combination of ECG, POCT troponin T (TnT) and TTE in a prehospital setting is not known. Technological improvements have made telemedical digital transmission of TTE images from ambulance paramedics to in-hospital cardiologists possible, thereby potentially improving the prehospital diagnostic precision in patients with chest pain.
The aims of the present study were to evaluate the feasibility and diagnostic accuracy of prehospital acquisition of the combination of ECG, POCT TnT and TTE by paramedics in identification of NSTEMI in patients with chest pain.
Methods
Study design
This prospective open-label non-randomised diagnostic accuracy study was conducted and reported according to the Standards for Reporting Diagnostic Accuracy (STARD) recommendations.16 The study was conducted at Sorlandet Hospital, Norway.
Study population
Consecutive patients ≥18 years of age requesting an ambulance from the local Norwegian Emergency Medical Communication Centre (EMCC) due to chest pain between November 2017 and January 2020 were screened for inclusion (figure 1). The dedicated study ambulance served a population of approximately 100 000 inhabitants, was located 67 km from a PCI hospital and was operational from 08:00 to 20:00 hours, 2–4 days/week. Patients with ST-elevation were excluded and transferred for primary PCI or treated with prehospital fibrinolysis according to current guidelines. Patients with haemodynamic instability and/or severe arrythmia requiring immediate treatment, conditions affecting the ability to cooperate and obvious non-cardiac origin of chest pain were also excluded.
Study flow chart. PCI, percutaneous coronary intervention.
Diagnostic devices
One emergency medical system ambulance was equipped with a Lifepac 15 (Physio-Control, Washington, USA) ECG recorder. ECG recording from patients with chest pain and transfer to an in-hospital cardiologist are routine in all ambulances in the region. No separate training was given due to this study.
A Cobas h232 device (Roche Instr, Switzerland) for prehospital analysis of POCT TnT was mounted in the ambulance. The measuring range was 40–2000 ng/L. Hospital laboratory staff trained paramedics in blood sampling and POCT TnT analysis, and performed quality control, temperature control and monthly calibration of the device.
A laptop-sized ultrasound scanner (Vivid IQ with M5Sc-RS probe, General Electric Healthcare, Horten, Norway) with a mobile broadband connection to a General Electric EchoPac server at the hospital, was fixed in a bracket next to the stretcher in the ambulance. Six paramedics with no previous experience in performing ultrasound examinations were trained in standard B-mode TTE image acquisition (parasternal long axis, parasternal short axis, apical four chamber, apical two chamber and apical long axis) in healthy volunteers. The training was perfomed over 2 days by a cardiologist and an echo sonographer. The training included handling of the ultrasound probe, selection of probe positions, basic education in anatomy of the heart in relation to imaging views, optimisation, selection and storage of adequate images and digital transfer of images. No training was provided in the use of Doppler methods, and no image analyses were performed by the paramedics. Simulation scenarios were conducted prior to the first dispatch, and an echo sonographer participated with practical instructions and guidance in real patient situations over 3 days in the beginning of the study period.
Study procedure
The study ambulance was dispatched by the EMCC according to the Norwegian Index for Emergency Medical Assistance criteria to patients with chest pain.
A 12-lead ECG was obtained by ambulance paramedics at first medical contact (FMC). The ECG was digitally transmitted and interpreted by the hospital cardiologist on duty.
POCT TnT was analysed in the ambulance after first intravenous access, and the result was communicated to the in-hospital cardiologist by telephone.
TTE was performed in the ambulance before site departure, with the patient on the stretcher facing 45 degrees left towards the paramedic. Image acquisition of the five standard TTE projections were stored, transferred and immediately assessed by the in-hospital cardiologist. The cardiologist’s evaluation of RWMA was based on visual analysis of all myocardial segments, assessing normokinesia (normal wall thickening and endocardial excursion), hypokinesia (reduced wall thickening and reduced endocardial excursion), akinesia (absence of either wall thickening or endocardial excursion) and dyskinesia (systolic outward stretching or thinning) in any projection. Wall motion score index was not systematically calculated. TTE image quality was scored by the cardiologist on duty on a five-level Likert-type scale based on the proportion of interpretable myocardial segments (1: no myocardial segment interpretable; 5: all myocardial segments interpretable).
Further action was determined by the cardiologist in real time by evaluating the information (history/symptoms, ECG, POCT TnT and TTE) provided by the paramedics. NSTEMI was presumed in patients with new ischaemic ECG findings, elevated POCT TnT and/or new RWMA at TTE. Patients with suspected NSTEMI were transported directly to the PCI hospital. The remaining patients were admitted to the local ED or referred to the primary healthcare service in accordance with standard ambulance protocols.
Information on gender, age, cardiovascular risk factors, previous cardiovascular diseases, symptoms, clinical findings, treatment strategy and complete time sets from first EMCC call to coronary angiography and PCI were registered in an electronic case report form by paramedics and cardiologists. Dispatch times for FMC, ambulance arrival, departure and hospital arrival were extracted directly from the ambulance registry. Medical note review was performed 90 days after index event, registering in-hospital assessment, treatment, discharge diagnoses, hospitalisation due to ACS at Sorlandet Hospital and death (according to the Norwegian population registry) during follow-up.
Outcomes
The feasibility end point was the proportion of patients with interpretable results of the ECG, POCT TnT and TTE tests. The diagnostic accuracy end point was the proportion of patients correctly diagnosed with NSTEMI in the prehospital setting. The prehospital diagnosis of possible NSTEMI was based on minimum one positive test (ischaemic ECG changes, elevated POCT TnT or RWMA at TTE). The discharge diagnosis was based on in-hospital diagnostics according to the third universal definition of MI.17
Patient and public involvement
No patients were involved in the design of this study.
Statistics
Continuous variables are presented as means±SD or medians (IQR) and differences between groups were analysed using independent samples t-tests. Categorical variables are presented as numbers and percentages. Sensitivity, specificity, negative and positive predictive values and accuracy are reported as percentages with 95% CIs. A final diagnosis of NSTEMI was used as reference standard. Missing or uninterpretable results are given for each diagnostic method. Sample size of 24–50 have been recommended for feasibility studies.18 Sample size calculation (n=245) for diagnostic accuracy was based on an estimate of the incidence of NSTEMI in the chest pain population (0.2), as well as assumed combined sensitivity and specificity for ECG, TnT and TTE (0.85), with beta ≤0.2. A p value of <0.05 was regarded as statistically significant. The data were analysed using STATA V.16 (StataCorp, College Station, Texas, USA). Summary statistics for diagnostic tests and sample size estimation were conducted with the user-developed commands ‘diagt’ and ‘diagsampsi’, respectively.
Results
A total of 253 patients were included during the study period from November 2017 to January 2020 (total operating days: 282). The average inclusion rate was approximately one patient per 12-hour shift.
A total of 151 (60%) patients were male and mean age was 61 (±17) years. Clinical characteristics and prehospital findings are presented in table 1. Median response time from emergency call to arrival of ambulance paramedics to patient location was 18 (IQR 12, 30) min. The total time from ambulance arrival to departure from patient location was median 46 (IQR 38, 56) min.
Clinical characteristics and prehospital findings in study patients with and without non-ST-elevation myocardial infarction (NSTEMI) requesting ambulance due to chest pain, Sorlandet Hospital 2017–2020
NSTEMI was the discharge diagnosis in 22 (9%) patients.
Feasibility
ECG was successfully recorded and transmitted from the ambulance to the hospital cardiologist in all 253 patients. The ECG was interpreted by the hospital cardiologist on duty in 243 (96%) patients and median time delay from FMC to ECG recording was 10 (IQR 7, 22) min. None of the patients without an interpreted ECG prehospitally had ST-elevation in the ECG at the hospital.
POCT TnT was analysed without practical or technical difficulties in 238 (94%) patients. Low ambient temperature and difficulties in providing venous access were the reasons for the lack of POCT TnT analysis in the rest of the cases. Median time from FMC to POCT TnT result was 21 (IQR 13, 34) min.
Prehospital TTE images were transferred to a hospital cardiologist in all patients. Median duration of prehospital TTE image acquisition and transfer was 11 (IQR 8, 16) min. Mean TTE image quality score was 3.6 (95% CI 3.5 to 3.7) out of 5. Median duration of cardiologist interpretation was 4 (IQR 3, 6) min. The TTE images were not possible to interpret due to poor technical quality in 13 (5%) cases. The paramedics reported difficulties in image acquisition of the standard TTE projections in 12 of these 13 patients. Patients without interpretable TTE were of similar body mass index to those with interpretable images (28 vs 27 kg/m2, p=0.43) and chronic obstructive pulmonary disease was reported in two patients without interpretable TTE images. None of the patients with non-interpretable TTE images had a NSTEMI.
Prehospital diagnosis of possible NSTEMI versus no possible NSTEMI based on an interpreted ECG, POCT TnT result and interpretable TTE images was possible in 217 (86%) of the study patients.
Diagnostic accuracy
Prehospital findings at ECG, TnT and RWMA at TTE are presented in table 2. ST-depression was the most common recorded ischaemic ECG change and was present in five (71%) of the seven patients with ischaemic ECG changes and NSTEMI. Median TnT value was 125 ng/L (range 51–410 ng/L) in patients with NSTEMI, while the TnT value ranged from 65 to 416 ng/L in the 10 patients with elevated TnT and no NSTEMI. Fifteen (79%) of the 19 patients with RWMA and no acute MI had a history of prior MI.
Prehospital findings at ECG, point-of-care troponin T and echocardiography in study patients with and without non-ST-elevation myocardial infarction (NSTEMI) requesting ambulance due to chest pain, Sorlandet Hospital 2017–2020
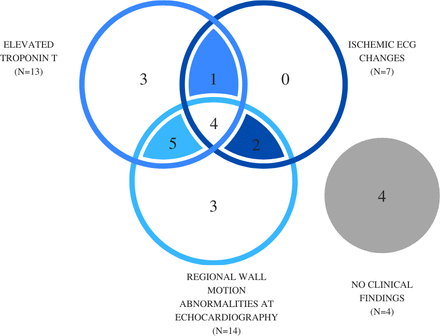
Four (18%) patients with NSTEMI had no ischaemic ECG changes, negative TnT and no RWMA at TTE. Six (27%) patients with NSTEMI had positive findings at one diagnostic method, eight (36%) patients had positive findings at two and four (18%) patients had positive findings at three of the diagnostic methods (figure 2). In three patients (14%) with NSTEMI, RWMA was the only positive test.
Elevated troponin T, ischaemic ECG changes and regional wall motion abnormalities at echocardiography in patients with non-ST-elevation myocardial infarction (n=22).
NSTEMI was correctly diagnosed prehospitally in 18 of 22 (82%) patients with NSTEMI.
The diagnostic utility of ischaemic ECG changes (ST-segment depression and/or T-wave inversion), elevated TnT (>50 ng/L) and RWMA at TTE in prehospital identification of NSTEMI in this study is presented in table 3.
Diagnostic utilities of ECG, point-of-care TnT and echocardiography in prehospital identification of non-ST-elevation myocardial infarction in study patients requesting ambulance due to chest pain, Sorlandet Hospital 2017–2020
A total of 50 (20%) patients without acute ischaemic ECG changes, elevated POCT TnT or new RWMA were further examined and treated by a general practitioner/emergency service after the assessment by paramedics and were not admitted to any hospital. None of these died or was admitted to Sorlandet Hospital for the next 90 days due to ACS. A total of 173 (68%) patients were admitted to the nearest local hospital, whereas 30 (12%) patients were transported directly to the PCI hospital. NSTEMI was diagnosed in 6 (3%) patients admitted to the local hospital and in 16 (53%) patients admitted to the PCI hospital. Two patients admitted to the PCI hospital had a discharge diagnosis of Takotsubo cardiomyopathy. A diagnosis of NSTEMI was suspected prehospitally in both patients.
A total of 21 (95 %) patients with NSTEMI underwent coronary angiography during hospitalisation. Median time from FMC to coronary angiography were 137 (IQR 96, 118) min in patients with NSTEMI admitted directly to the PCI hospital and 1147 (IQR 160, 1343) min in patients with NSTEMI admitted to the local hospital. Coronary angiography revealed total occlusion of the infarct-related artery in five (24%) cases. Three of these patients had RWMA at prehospital TTE, two patients had elevated POCT TnT and one had prehospital ischaemic ECG changes. In two of these five cases, RWMA at TTE was the only positive prehospital diagnostic test. Four patients with NSTEMI and occluded infarct-related artery were admitted directly to the PCI hospital.
Discussion
This study evaluating the feasibility and diagnostic accuracy of ECG, POCT TnT and TTE in prehospital identification of NSTEMI in patients with chest pain confirmed that paramedics could acquire and transfer ECG, POCT TnT and interpretable TTE images in most cases. Based on these examinations, it was possible by cardiologists to identify the majority of cases with NSTEMI prehospitally, and admit those patients directly to a PCI hospital for further treatment.
Prehospital 12-lead ECG recording with automatic transmission to hospital physicians has been a cornerstone of treatment strategy in patients with ACS in the Norwegian ambulance service system since the mid-1990s. This study confirms the inadequacy of ECG in risk stratification of patients with MI without ST-elevation, which constitutes >70% of the MI cases.6 19 The positive and negative predictive value of ischaemic ECG changes in this study were 37% and 94%, resepectively. Consequently, the majority of patients with NSTEMI have limited benefit of the prehospital ECG evaluation.
Prehospital POCT TnT measurement was technically feasible with short time usage in most patients. TnT had high sensitivity for NSTEMI, but >40% of the patients with NSTEMI presented with prehospital POCT TnT values below measuring range of the device (<40 ng/L). This emphasises the time-dependency and cut-off value limitations of prehospital POCT TnT.20 TnT usually rises within 1 hour from symptom onset and remains elevated for several days.21 Although a negative test cannot exclude MI, this study verified that POCT TnT is easy to implement and may be a useful adjunctive in the prehospital risk stratification of patients with chest pain.
Use of echocardiography is usually reserved for cardiologists and sonographers, and RWMA evaluations are an advanced TTE skill.22 In this study, we evaluated a combination of TTE image acquisition performed by paramedics in the prehospital setting and TTE image interpretation performed by in-hospital cardiologists. The proportion of interpretable examinations was high and the image quality was rated as acceptable in most cases. TTE image acquisition caused a relatively short prehospital delay (median 11 min). Isolated RWMA had limited sensitivity for NSTEMI in this study (64%), but adds an important contribution to the selection of treatment strategies, especially in patients with NSTEMI and occluded infarct-related artery. RWMA is more frequent in NSTEMI with total occlusion of a coronary artery.10 23 Prehospital TTE is an equipment, resource, competence and time-consuming method. If this is to be used routinely in the future, dedicated personnel and a high number of procedures are required. More advanced methods for assessing myocardial function by echocardiography, such as strain, may also improve the sensitivity.13 In the future, optimised image acquisition and automated image analysis using artificial intelligence might aid TTE for non-experts.
Two patients with suspected NSTEMI prehospitally had a discharge diagnosis of Takotsubo cardiomyopathy. Takotsubo cardiomyopathy may have symptoms and findings (ischaemic ECG changes, elevated TnT and RWMA at TTE) identical to MI, but is by definition not an MI.24 Nevertheless, prehospital identification is important for early diagnostic clarification.
An interesting and unexpected observation in the study was the large proportion of patients not admitted to a hospital after the assessment with ECG, POCT TnT and TTE. The negative predictive value of these tests were high, and the safety of this choice was supported by the fact that none of these patients died or was admitted to Sorlandet Hospital with ACS for the next 90 days. New diagnostic tools in the ambulance service might therefore contribute to avoid unnecessary hospitalisations.
This study has several important limitations. It is based on relatively few patients and covers a limited geographical area. The low inclusion rate might be a source of selection bias, as pronounced symptoms might be easier to recognise. The number of paramedics and cardiologists involved was also limited. Follow-up relied on information from the Norwegian population registry and clinical note review at the study hospitals. Any admissions to other hospitals were not registered. Generalisation of the findings to other ambulance systems and hospitals must be done with great caution. The patient’s age, symptoms and cardiovascular risk factors have probably had an impact on the choice of treatment strategy, but evaluation of this was beyond the scope of the study. Furthermore, the TTE images were only assessed during the initial consultation and were not retrospectively reviewed by independent cardiologists.
Conclusions
Prehospital risk stratification with ECG, troponin and TTE in patients with suspected NSTEMI is feasible in collaboration between trained paramedics and cardiologists. These diagnostic modalities in combination had a high diagnostic accuracy for the diagnosis of NSTEMI. However, a larger study with a control arm is needed to further determine the diagnostic accuracy and evaluate the impact on morbidity and mortality after MI.
Abstract translation
This web only file has been produced by the BMJ Publishing Group from an electronic file supplied by the author(s) and has not been edited for content.Data availability statement
Data are available on reasonable request. The data that support the findings of this study are available on request from the corresponding author (JJ). The data are not publicly available due to state restrictions.
Ethics statements
Patient consent for publication
Ethics approval
The Regional Committee for Medical and Health Research Ethics approved this study (REK 2017/701). All study participants signed a written consent form at time of inclusion in the study ambulance.
References
Supplementary materials
Supplementary Data
This web only file has been produced by the BMJ Publishing Group from an electronic file supplied by the author(s) and has not been edited for content.
Footnotes
Handling editor Edward Carlton
Correction notice This article has been corrected since it was first published. The open access licence has been updated to CC BY.
Contributors JJ is responsible for the overall content as guarantor. JJ accepts full responsibility for the finished work and the conduct of the study, had access to the data, and controlled the decision to publish. LJ and JJ were responsible for the conception of the study and the analysis and interpretation of the data. LJ and JJ drafted the manuscript. BG and RBO contributed to the interpretation of the data and the revision of the manuscript. All authors gave final approval and agreed to be accountable for all aspects of this work, ensuring its integrity and accuracy.
Funding The Norwegian Air Ambulance Foundation was the main sponsor of the project. General Electric Healthcare provided the telemedicine solution and gave support free of charge. The South-Eastern Norway Regional Health Authority provided financial support for telemedicine solution development through an innovation grant.
Disclaimer The funders had no role in the design and conduct of the study, in the collection, analysis and interpretation of the data, and in the preparation, review or approval of the manuscript.
Competing interests None declared.
Patient and public involvement No patients were involved in the design of this study.
Provenance and peer review Not commissioned; externally peer reviewed.
Supplemental material This content has been supplied by the author(s). It has not been vetted by BMJ Publishing Group Limited (BMJ) and may not have been peer-reviewed. Any opinions or recommendations discussed are solely those of the author(s) and are not endorsed by BMJ. BMJ disclaims all liability and responsibility arising from any reliance placed on the content. Where the content includes any translated material, BMJ does not warrant the accuracy and reliability of the translations (including but not limited to local regulations, clinical guidelines, terminology, drug names and drug dosages), and is not responsible for any error and/or omissions arising from translation and adaptation or otherwise.